Foot Arch Pain
Types of Foot Arch Pain, Causes, Symptoms & Treatments
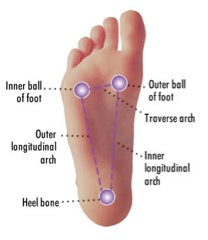
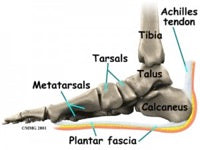
Let’s begin with a definition of the arch of a foot. The arch is composed of the tarsal and metatarsal bones of the foot, which are strengthened by tendons and ligaments. These form a band of thick tissue known as the plantar fascia stretches from the toes to the heel of the foot, connecting these bone structures. The plantar fascia is important for such mechanical elements as:
- Enabling the foot to bear weight more weight without injury
- Supporting the arch of the foot
- Absorbing shock
- Working like a spring to elongate one’s gait
Arch pain and other types of foot pain usually stem from something being out of whack in either the function or the interaction of the structures of the foot, be it due to a foot arch injury, a neurological condition or a hereditary structural abnormality. This often causes inflammation, and inflammation typically results in arch foot pain.
With these basics covered, I will now delve into some of the causes of the arch of foot pain and what one can do about it.
Plantar Fasciitis Foot Pain: Arch and Heel
Plantar fasciitis is a condition that typically causes pain in the heel, but for some, this can also coincide with pain in the arch of the foot. Plantar fasciitis occurs when too much tension is placed on the plantar fascia, resulting in small tears. Over time, repeated tearing and stretching of this tissue causes inflammation and thus pain in foot arch.
This foot pain in the arch is usually most evident with one’s first steps after getting out of bed or upon moving after a period of inactivity. Climbing stairs or standing for a long stretch of time is often associated with especially sharp pain in the arch of the foot or the heel due to plantar fasciitis.
There are a number of causes of plantar fasciitis, including obesity and pregnancy, wearing unsupportive shoes, careers that require one to spend extended periods of time standing on hard surfaces and structural abnormalities of the foot. Certain activities that put inordinate amounts of stress on the plantar fascia, such as ballet or distance running, are also associated with arch pain in the foot.
Plantar fasciitis treatment typically involves wearing a night splint to stretch the plantar fascia while one is sleeping and the use of a foot pain arch support to help distribute pressure more evenly across the foot. Besides orthotics, one can also engage in foot massages and stretches in addition to avoiding or cutting back on the irritating activity. Icing the foot can also help reduce inflammation and achieve foot arch pain relief.
High Arches Foot Pain
As alluded to in the previous section, foot pain in the arch can also stem from an abnormally high foot arch or pes cavus. In an estimated 50% of cases, high arches are caused by a hereditary neuromuscular condition is commonly known as Charcot Marie Tooth (CMT) disease.
Outside of this, high arch foot pain is not well understood; it is thought to stem from a variety of neurological, orthopedic, or neuromuscular conditions, ranging from a post-trauma malformation of the bone to an shortening of the Achilles tendon to muscle weakness.
Symptoms of high arches include trouble fitting into shoes and arch of the foot pain while walking, running or standing. If left untreated, this can result in chronic pain as well as permanent trouble walking or running.
Treatment of pain in the arch of the foot due to high arches typically involves the use of orthotics, such as corrective shoes, arch inserts of supportive insoles to help more evenly distribute force across the foot and to reduce the amount of strain on the plantar fascia. Stretching and engaging in strength exercises for the muscles of the foot can also be helpful toward foot arch pain treatment. Surgery is typically only pursued in instances of sharp pain in foot arch that does not respond to more conservative modes of treatment.
Foot Pain: Fallen Arches & Flat Feet

The opposite of high arches—a fallen arch or flat foot—can also be causes of pain in the arch of the foot. Whereas flat feet are generally structural issues that are present from birth, a fallen arch is an acquired condition resulting from a change in the posterior tendon that is responsible for supporting the arch of the foot and providing stability for walking. Thus, fallen arches are more scientifically known as posterior tibial tendon dysfunction. This tendon starts at the calf and stretches along the inner part of the leg to attach to the bones on the inside of the foot.
For some, pain in the foot arch due to posterior tibial tendon dysfunction occurs gradually over time simply due to the wear and tear of daily life. This can be accelerated by overusing the feet, participating in high-impact sports or wearing shoes with poor support. Foot arch injuries can also lead to a fallen arch, such as a fall or other such trauma.
Certain activities also increase the risk of this type of foot pain in the arch of the foot, including obesity, diabetes, steroid injections or high blood pressure. Fallen arches are also more common among women and those over the age of 40.
The symptoms of fallen arches include pain under the arch of the foot that worsens with activity or when walking on uneven ground, as well as swelling of the inner part of the ankle. As a result, people with fallen arches often have trouble walking or standing for long periods of time.
If nothing is done to address the injury, the tendon will start to degenerate and pain will move to the outside of the ankle as the heel bone will begin to shift outward. This condition can also cause pain in the knees or back due to the less-than-ideal leg alignment that results.
If one catches this injury early, it can usually be treated via non-invasive methods such as cutting back or stopping the problematic activity or switching to a sport that involves less impact, icing the foot, taking non-steroid anti-inflammatory drugs (NSAIDs), losing weight (if applicable) and wearing a short cast, walking boot or some other orthotic that controls foot position to stabilize the tendon.
Tarsal Tunnel Syndrome Foot Pain: Arch
The posterior tibial nerve can also be pinched or entrapped as it travels through the flexor retinaculum, which is a supportive band along the inner part of the ankle, a condition known as tarsal tunnel syndrome (AKA, posterior tibial neuralgia). This might occur due to an ankle injury or if one’s ankle tends to roll inwards when walking or running. Things that put pressure on the tarsal tunnel, such as the formation of a cyst or inflammation of the tibial tendon can also cause tarsal tunnel syndrome.
This type of injury typically causes pain in the ankle, but this can affect the arch or the entire foot. The pinched nerve can also cause weakness, numbness, tingling or burning pain in the arch of foot or ankle. This pain, tingling, numbness or burning sensation can also radiate up the leg all the way to the knee and it typically worsens with activity.
Treatment of tarsal tunnel syndrome typically involves following the steps of RICE (rest, ice, compression, and elevation), engaging in strengthening physical therapy, wearing orthotics, such as a walker boot, taking anti-inflammatory medications and in some cases getting corticosteroid and anesthetic injections. If these fail, tarsal tunnel release surgery may be necessary.
Psoriatic Arthritis Pain: Arch of Foot
Psoriatic arthritis is an inflammatory form of chronic arthritis. It occurs when the body’s immune system attacks healthy cells and tissue, causing inflammation of the joints and excess production of skin cells. This causes the fingers or toes to swell up like sausages and can cause pain or stiffness where the ligaments or tendons of the body, especially where they attach to the bones of the foot (as well as other areas of the body), such as the ball of the foot. Psoriatic arthritis is also associated with changes to the nails and fatigue.
But what causes this atypical immune system response is not well understood—it is thought to stem from both genetic and environmental factors. It is often associated with a family history of the condition or having psoriasis and it typically affects those between the ages of 30 and 50. Trauma or infection can trigger psoriatic arthritis in those with an inherited predisposal toward it.
Unfortunately, there is no cure for psoriatic arthritis. Therefore, treatment of this form of arthritis revolves around reducing and controlling the inflammation via NSAIDS in mild cases. Some doctors might recommend of corticosteroid injection into the joint or in cases where the condition has progressed to major joint destruction, surgery. Conservative modes of self-help involve the use of ice or heat packs and maintaining a healthy weight and level of physical activity.
Plantar Fibromatosis Pain: Foot Arch
Plantar fibromatosis is a rare condition characterized by the thickening of the plantar fascia and the formation of non-cancerous nodules or cords on the tissue. These nodules, known as fibromas, are usually slow-growing, but eventually, they can cause pain under foot arch when the nodules rub against the floor and they can make it difficult for one to the toes. A visible lump that is firm to the touch is another symptom of plantar fibromatosis. This condition usually occurs on the medial part (inner) of the foot near the highest point of the arch.
The cause of this condition is not well understood, but some generalities can be made. It is more common in Caucasian males, especially those over the age of 70. There is often a family history of this condition. Overuse of the feet over an extended period and some sort of trauma to this region of the foot are also linked to the formation of plantar fibromatosis. Other conditions that are considered risk factors for the disease include:
- Diabetes mellitus
- Epilepsy (seizure medicine)
- Palmer fibromatosis
- Peyronie’s disease
- Thyroid problems
- Liver disease
- Alcoholism
In cases where the nodules are small and minimally painful, treatment typically involves easing the pressure on the fibroma via shoe inserts, night splints, heel cushions or arch supports. In more severe cases, a cortisone injection or surgery may be necessary.