Plantar Fasciitis: The Complete Guide
In my opinion, getting out of bed in the morning in and of itself is an unpleasant task, so my heart goes out to those suffering from plantar fasciitis, a condition whose symptoms include a stabbing sensation in the heel that often coincides with the first steps of the day. This pain may also flare up when you begin moving around after sitting or after engaging in an intense activity.
What Is Plantar Fasciitis?
The condition’s name is derived from the plantar fascia, which is the thick tendon that connects your heel and your toes, creating the arch in your foot. Extra pounds, non-supportive shoes, long periods standing on hard surfaces and certain athletic activities that put a lot of stress on that region of the foot, such as ballet or distance running, can cause this tendon to tear and become irritated, which leads to sharp pain in the heel.
Plantar fasciitis is a condition characterized by a stabbing sensation in the heel that most often accompanies the first steps of the day. Once one has moved around a bit, limbering up the foot, the pain typically eases. Similarly, the stabbing sensation may also flare up when one stands after sitting for an extended time. The pain may also return following long hours on the feet or after an intense bout of physical activity.
What Causes Plantar Fasciitis?
Plantar fasciitis takes its name from the tissue that causes the painful condition. The plantar fascia is the thick tissue at the bottom of the foot that connects your toes to your heel bone and creates the arch in your foot.
The Mayo Clinic likens the plantar fascia to a bowstring that absorbs shock and supports the arch of one’s foot. If the tension becomes overbearing, small tears may form in the ligament. Repetitive tearing or stretching of the tissue inflames and irritates the fascia and causes the painful sensation in the heel.
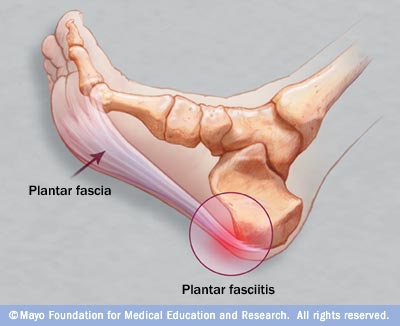
Plantar fasciitis is a condition that develops gradually over time, and it typically (though not always) affects just one foot.
Who Suffers from Plantar Fascitis?
This condition is more common among women and those between the ages of 40 and 60. It is also more prevalent among people who are overweight or pregnant. Those engaging in activities such as ballet or distance running are also more likely to suffer from plantar fasciitis as these activities put more stress on the heel and related tissues. Those who spend long hours standing on hard surfaces (e.g., teachers, hairdressers, soldiers) are also more likely to suffer from plantar fasciitis.
Those who have flat feet, high arches or an abnormal way of walking are more prone to this condition. Plantar fasciitis is also more prevalent among people whose shoe collection resembles mine, which is dominated by soaring heels (I tend to overcompensate for my short stature), a few thin-soled flats, and a multitude of fluffy, loose-fitting slippers. The common denominator is that they do not provide adequate support.
thankfully, most cases of plantar fasciitis can be treated via relatively conservative methods, including staying off your feet, stretching the arches, icing the foot, adding orthotic plantar fasciitis insoles to your shoes and wearing night splints to promote healing while you are sleeping.
Physical therapy aimed at strengthening your feet and lower calves can also improve the distribution of pressure across your feet, providing plantar fasciitis relief and helping to prevent another flare up.
Anti-inflammatory pain relievers can be taken for pain relief or cortosteroids may be applied via injection or as a solution to the affected region. In more extreme cases, shockwave therapy or surgery may be considered.
To learn more about plantar fasciitis symptoms, causes, treatment and prevention, visit BraceAbility’s extensive resource library with many articles about foot conditions like Plantar Fasciitis. BraceAbility also carries a complete line of orthotics for Plantar Fasciitis to help alleviate your plantar pain without undergoing surgery.
Foot Plantar Fasciitis Treatment
Thankfully, the vast majority (90%) of plantar fasciitis cases can be treated by relatively noninvasive methods in a matter of months. But it is very important to seek treatment because if this condition is left unattended, it will likely alter one’s way of walking, which can then manifest into problems with other areas of the foot, knee, hip or back.
For the pain, doctors typically prescribe nonsteroidal anti-inflammatory drugs, which is a fancy way of saying pain relievers such as Aleve or ibuprofen. Another drug that is used for treating an inflamed plantar fascia is cortosteroids, which are usually applied as a solution that is absorbed with the help of electric current, though this can also be administered via injection.
Another way of addressing the problem and preventing it from reoccurring is taking part in physical therapy aimed at stretching the affected areas of the foot and strengthening the lower region of the leg to improve the stability of your foot and ankle.
Orthotics for Plantar Fasciitis Pain
Arch supports (AKA, orthotics for plantar fasciitis) may also be worn to help distribute pressure more evenly across the foot.
A therapist might also recommend wearing night splints as a remedy for plantar fasciitis. These splints treat the condition while the user is sleeping by stretching the Achilles tendon and calf muscles. BraceAbility offers several night splints for plantar fasciitis treatment.
Some more extreme methods of treating plantar fasciitis include shockwave therapy to stimulate healing, and when all else fails, one may undergo surgery to remedy the situation.
Chronic Plantar Fasciitis Prevention
Most at-home remedies and prevention techniques are fairly common sense when one considers the causes of plantar fasciitis. Staying off one’s feet for a few days to give the plantar fascia a chance to heal can be helpful, as can foot massages, arch stretches and icing the affected region.
If the injury is due to sports, one should cut back on the distance or amount of time spent on athletic activities that are particularly stressful to the heel and perhaps even a switch to lower-impact sports, such as swimming. Maintaining a healthy weight also limits one’s chances of suffering from plantar fasciitis.
As previously mentioned, adding arch supports to one’s shoes can provide relief. It is also important to replace athletic shoes in a timely fashion and to wear shoes with good support.