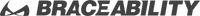Everything You Ever Wanted to Know About Scheuermann’s Disease… from Schmorl’s Nodes to Bracing to Surgery
This mouthful of a condition is named after the Danish radiologist who first “discovered” (described) the issue affecting juveniles’ spines back in 1921, Holger Scheuermann.
Scheuermann’s Disease, sometimes mispronounced “Sherman’s Disease,” goes by many names, including Calve Disease, juvenile osteochondrosis of the spine, juvenile disc disorder, juvenile discogenic disorder, and Kelso’s hunchback, to name a few.
What Is Scheuermann’s Disease?
Scheuermann’s Disease is a developmental disorder of the spine that is caused by abnormal growth of the vertebrae. Specifically, the outer part of the vertebra grows at a normal rate, while the inner part of the bone grows more slowly. This results in anterior wedging of the vertebrae.
Who Does It Affect?
It typically affects young people, striking during the growth spurt just before puberty. But this condition is not something that simply goes away once you’re done growing. Therefore, many adults suffer from old cases Scheuermann’s kyphosis as well.
Some studies have shown it has no gender association, but others have indicated it may be more common with boys than girls. Mayo Clinic is one particularly reputable source that says boys are affected more often than girls.
Scheuermann’s syndrome is thought to affect somewhere between 4% and 8% of the general population and it is the second most common cause of back pain in children after spondylolysis with spondylolisthesis, according to American Journal of Physical Medicine & Rehabilitation.
It occurs in children who are otherwise normal and healthy.
What Does Scheuermann’s Disease of the Spine Look Like?
Typically, this occurs in the upper, thoracic vertebra (specifically the T7-T10 vertebrae), though there are cases of lumbar Scheuermann’s Disease.
While upper back incidences of this wedge deformity of the spine are far more common, lumbar wedging caused by Scheuermann’s Disease in the lower back causes more pain, limited mobility and is more likely to continue into adulthood.
The result of this thoracic disorder is the spine curves more than it should, resulting in what is defined as dorsal kyphosis, or a hunched back.
Note that this is quite different than postural kyphosis. Humped backs where poor posture or weak muscles are to blame can be corrected if an individual makes a conscious effort to do so.
Since Scheuermann's kyphosis is due to structural changes to the spine (specifically, wedging of the anterior vertebrae), the curve cannot be straightened.
This makes it more similar to degenerative kyphosis related to aging and arthritis, though they clearly affect people at different ends of the age spectrum.
Scheuermann's Disease Radiology
A normal human’s thoracic spinal curve falls somewhere between the range of 20 degrees and 50 degrees. Curves greater than 50 degrees typically signal some sort of spinal problem, like Scheuermann’s kyphosis.
As you might imagine, the overly curved nature of the spine can cause issues with the cushioning between the vertebrae and some of the disc may even push into the vertebrae, creating a “Schmorl’s node.”

Descriptions of Schmorl’s nodes note they generally do not cause many problems and they are in fact a pretty common side effect of general wear and tear on the spine. The difference in this scenario, of course, is that they are showing up in children.
Two Main Types of Gibbus Deformity
There are two main types of Scheuermann's syndrome, based on the location of the wedging/increased convexity of the spine (AKA, Gibbus deformity). They are divided as follows:
- Apex at the mid-thoracic level (T7-T9)
- Apex at in the thoracolumbar junction (T11-T12)
What Causes This Form of Osteochondrosis?
Unfortunately, the cause of this condition is unknown, though most experts say several factors are likely at play. Some possible risk-factors include:
- Juvenile osteoporosis
- Malabsorption
- Infection
- Endocrine disorders
- Biomechanical factors like a shortened sternum
- Injury to a bone or weakness before puberty
Scheuermann's Disease is also thought to have a hereditary/genetic link, though the inheritance pattern is also unclear.
What Are Some Scheuermann's Disease Symptoms?
- Pain in the thoracic spine and surrounding areas (most common symptom)
- Increased bend of mid/upper back (AKA, kyphosis)
- Neck pain
- Restricted movement, especially the ability to bend backward
- Discomfort that’s heightened by activities requiring a lot of twisting, bending or arching or long days sitting or standing
- Tiredness, muscle stiffness, especially after a long day sitting in class
- Redness on the skin where the kyphotic curve is most pronounced and rubs against chairbacks
- Muscle spasms, cramps
- Tight hamstrings
- Feeling off balance
- Excessive curve of the lumbar spine (the body’s natural way of compensating)
- Men with it tend to have broad, barrel chests (possibly to compensate for the loss of breathing depth)
- Large lung capacities
This thoracic spine disease also comes with the threat of complications, such as pressure on the nerve root and related neurological symptoms. In severe cases, it can also damage the spinal cord or internal organs, which can cause chest pain and heart and breathing issues down the road.
Also, around 20% to 30% of people with Scheuermann's Disease also have some degree of scoliosis.
Your child could also develop stress fractures in the low back due to the exaggerated lordosis that often comes along with kyphosis of the upper back.
While all of this can sound quite scary, know that for most people symptoms (besides the humpback of the thoracic spine) will ease once the spine is done growing. And while the round-back shape of the spine will not improve once skeletal maturity is achieved, it usually does not get worse, either.
So adverse sequelae stemming from Scheuermann’s kyphosis are limited for most.
Diagnosis of Scheuermann's Disease
A doctor will observe your child in a number of different positions, assessing both the curvature of the back and his or her range of motion from the front, back, and side, as well as while reclining.
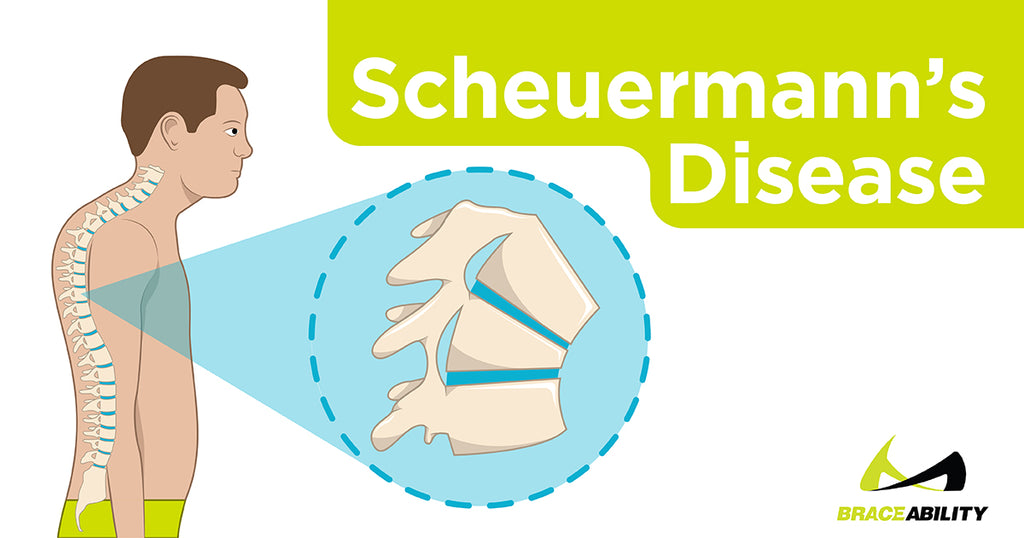
An Adams test is a part of the differential diagnosis process that can help distinguish Scheuermann kyphosis from postural kyphosis. For an adolescent with postural kyphosis, the curve of the back will generally smooth when he or she bends forward. That is not the case when Scheuermann’s kyphosis is to blame for the hump. This is one of those cases where a picture does a far better job of explaining the test than any dictionary description.
An X-ray of the spine typically shows classic wedging of the vertebrae and Schmorl’s nodes. In some cases, a doctor may recommend an MRI that will show additional detail.
By medical definition, Scheuermann’s Disease is diagnosed if the curve of the spine is 45 degrees or more and at least three vertebrae are wedged together by at least 5 degrees per segment. That backbone wedge is an anterior wedge where the wider part of the vertebrae is outward, facing toward the skin of the back.
Other intervertebral osteochondrosis symptoms a doctor may notice during the exam include:
- Schmorl’s nodes
- Hyperlordosis of the cervical and lumbar spine
- A forward-head position
- Irregularity and flattening of vertebral endplates
- Narrowing of spaces between the discs
Scheuermann’s Disease Treatment
Early treatment of Scheuermann's kyphosis is essential for stopping it from becoming a lifelong disability with an expensive price tag.
Online forums are riddled with stories of adults who are now dealing with back pain and other issues because they were simply told to stop slouching during their childhood and teenage years because either their doctor or parents did not realize their kyphosis was more than a postural problem.
If you’re unsure, get your child (or yourself) checked out. There are things you can do as an adult to make living with Scheuermann’s kyphosis better.
Treatment Options
Generally speaking, there are three ways to treat this thoracic spine syndrome:
- Monitoring/exercise
- Bracing
- Surgery
If your child has just a slight spinal curve that does not appear to be worsening and little to no pain, it may be enough simply to monitor the curve with periodic x-rays. Physical therapy, home exercise and pain management methods (ice, anti-inflammatory pain meds, etc.) can help with any related discomfort or range of motion loss.
But bracing would likely be recommended for children/teens with at least a year of spinal growth left and a more advanced curve.
If the patient is skeletally mature, wearing a back brace will do little good, so treatment in that scenario would likely focus on pain management and therapy to improve the strength and flexibility of the back.
Scheuermann’s kyphosis surgery is an option of last resort that is only considered when vertebral wedging is pretty severe and/or kyphosis is compromising the function of internal organs. We’ll dig deeper into that later.
Manage Pain and Protect the Back
You may need to try a variety of methods to ease hunch back pain. Ice therapy can help lower any inflammation and heat therapy can ease strained muscles (this article can help you decide between heat and ice therapy).
Adding some extra pillows for the back can lead to a more comfortable night of sleep. And a doctor might recommend various medications for pain relief.
A physiotherapist also has a number of tools that can help, including electrotherapy, taping techniques, soft tissue massage, Scheuermann’s Disease exercises and various other ways of unloading inflamed structures. Some therapists are even trained in acupuncture.
Restore Flexibility and Strength
Once your child’s pain is under control, the focus can shift to improving the strength and flexibility of the muscles that control the posture of her back. You might be surprised to hear that includes the hamstrings and the entire core.
While Scheuermann’s kyphosis exercises will not correct the deformity, they can help improve your child’s comfort level and the function of the back.
Regular exercise can make the back more limber, ease pain and reduce fatigue. When used along with bracing for Scheuermann's kyphosis, it can also reduce the risk of needing surgery.
Undergoing physical therapy at a young age can also help prep your child for life, teaching him or her good posture practices, the importance of remaining physically fit and helping to limit the risk of problems later in life.
Some also stress the importance of a balanced diet for those with Scheuermann’s kyphosis, as some issues can be related to the spine not getting the nutrients it needs from food.
Good Exercises for Scheuermann's Disease
Lower-impact sports are a great option for those with an excessively round upper back. Some examples include aerobics, swimming, and cycling.
Bad Exercises for Scheuermann's Disease
On the flip side, high-impact sports involving a lot of jumping, physical contact or stress on the back are not a great idea for someone with Scheuermann’s kyphosis. For instance, gymnastics, hockey, and football may do more harm than good.
Someone with this condition should also avoid exercises that overload the thoracic spine, such as sit-ups or crunches.
Alternative Conservative Methods of Treatment
An adult with Scheuermann’s kyphosis or children with mild cases of this spine disorder where a full Milwaukee brace would be overkill might consider wearing a posture brace to keep the back in as much extension as possible.
Wearing a simple upper back brace for Scheuermann's Disease can act as a reminder to straighten the back as much as possible and to keep the shoulders rolled back.
Another physiotherapy option you might consider for juvenile kyphosis is the Schroth method. This German system of physical therapy treatment is specifically designed for patients with scoliosis and related spinal deformities (several of which also happen to start with an s) like Scheuermann’s Disease.
Other options for Scheuermann’s Disease care in adults, teenagers or children might include acupuncture, massage or chiropractic treatment. While these methods will not “cure” the atypical shape of the back, they may improve its function and ease pain.
But you should always consult a doctor before trying out alternative methods.
More on Using a Scheuermann's Kyphosis Brace
Wearing a brace for Scheuermann’s Disease during the growing years can help slow or stop the progression of the wedge deformity thoracic spine for your child, thereby reducing pain and the hump of the back. Indeed, some recent research even signals bracing may help once spinal growth is complete.
When to Wear a Brace for Humpback Disease
Bracing is generally considered as a treatment option when the kyphosis curve falls between 50 degrees and 70 degrees. For milder cases, the aforementioned treatment methods usually suffice. For more severe cases, surgery will likely be considered.
As previously mentioned, bracing is typically most effective when the orthotic is worn before spinal growth is complete and especially before your child reaches his rapid-growth phase.
He’ll have the best results if the brace is worn around the clock for a year or two—as prescribed by a Scheuermann’s Disease specialist, of course.
Traditionally, the go-to style of brace is a Milwaukee brace—a full-torso brace that extends from the pelvis to the base of the skull. It comes with three bars (two in the back and one in the front) that are attached to a pelvic girdle and a neck ring with a throat mold, as well as a rib pressure pad.
This configuration helps to limit the curve of the low back and reminds the patient to retract the chin, keeping the head centered over the pelvis.
But professionals are increasingly recommending sleeker kyphologic and TLSO-style braces for dealing with wedge-shaped vertebrae. Some studies have shown them to be equally effective as the larger, bulkier Milwaukee brace.

Best Practices for Using a Scheuermann's Disease Brace
For the best results, it’s important for your child or teen to care for the brace and follow usage instructions as closely as possible. Usually, that includes wearing the brace for 16 to 23 hours per day for around a year, and then at night for two years or until your child reaches full skeletal maturity.
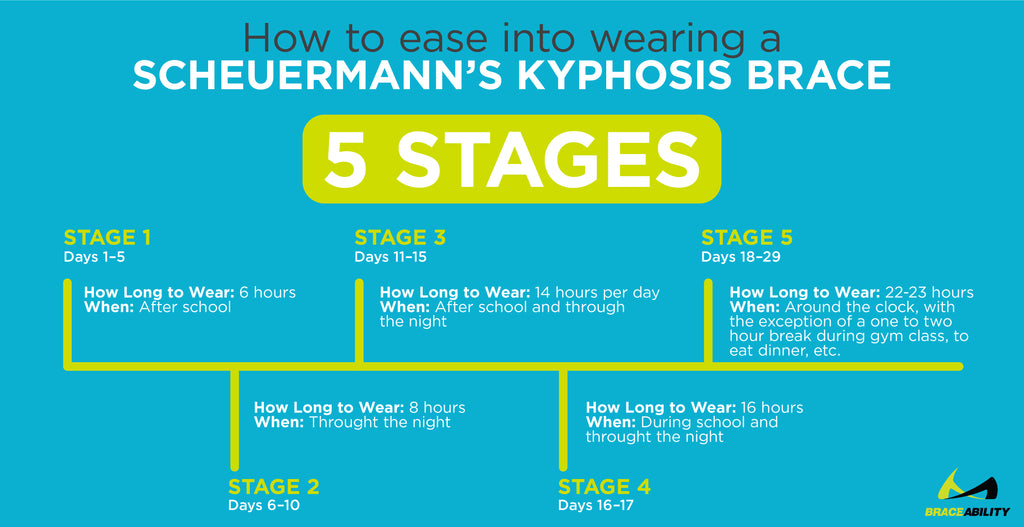
But you’ll need to ease into wearing back brace for a hunched spine. Professionals often recommend a five-stage process stretching over roughly 20 days for doing so.
- Stage 1, Days 1-5:
- Duration: 6 hours
- When: After school
- Stage 2, Day 6-10
- Duration: 8 hours
- When: Through the night
- Stage 3, Days 11-15:
- Duration 14 hours per day
- When: After school and through the night
- Stage 4, Day 16-17:
- Duration: 16 hours
- When: During school and through the night
- Stage 5, Day 18-29:
- Duration: 22-23 hours
- When: Around the clock, with the exception of a one- to two-hour break during gym class, to eat dinner, etc.
Help Your Child Put on the Brace:
At least in the early stages of brace-wearing, your child will likely need some help putting on his or her hunchback disease brace.
Follow the instructions for doing so carefully. And once the brace is on, check to see if it is applied correctly. That means there should be no pressure from the chin piece as your child sits or stands.
The pelvic portion of the brace should fit snugly. If it’s too loose, it will ride down over the pelvic bones, irritating the skin.
Don’t Rest the Head on the Chin Piece
Encourage your child to avoid resting against the chin piece for long periods. When reading a book or using a cell phone or iPad, your child will need to either get far enough way from the device/book that he/she can see it without looking down or use some sort of reading stand.
This can also present issues when eating. It can help to sit on a low stool or raise the height of the plate.
Stay Active—Whether the Brace Is On or Off
Wearing a back brace tends to produce lazy muscles, especially in the stomach and low-back area. Ironically, these core areas are very important for maintaining good posture.
So while it might be tempting to treat your child like he/she is breakable, know that its good for children with juvenile Scheuermann’s Disease to be active as any other kid.
Some activities like baseball and cycling can be done while wearing a brace for Scheuermann’s kyphosis.
And your child should make the most of her time free of the brace. During that one to two-hour stretch, she can do activities that require balance correction or flexibility like skating, snowboarding, skiing, ballet, or even bouncing around on a trampoline.
Swimming and other water sports are also great activities when your child is not wearing his or her brace.
About the only sports, you will want to avoid are those involving a lot of contact or high impact.
What to Wear Over/Under the Brace:
Many adolescents like wearing a snug, 100% cotton t-shirt or stockinet top under the brace. One thing to keep in mind when selecting such undershirts is to choose one with no wrinkles or seams, as these can irritate the skin.
Also know that your child may need to change the shirt several times a day, depending on the weather, activity level and how prone she is to sweating.
For clothing worn over the brace, you’ll likely need to go up a size from what your child typically wears.
Skin Care
While it might be tempting to use oily or greasy ointment/lotion on areas where the brace touches the skin (especially at first), don’t. Such materials soften the skin and can actually lead to more skin breakdown.
A better option is to keep the skin clean and dry and possibly to use rubbing alcohol on pressure areas to toughen the skin a bit.
It’s also important that your son shower or bathe every day, at which point he should also check for red, sore or raw areas. If these occur, he shouldn’t wear the brace until the raw spot heals.
Know those repeat problems likely mean the brace either doesn’t fit correctly or that it isn’t being worn properly.
Take Care of Your Brace
A clean, well-cared for brace will save you money and make for a better experience in the long-run. Periodically check the orthotic for loose screws and tighten them as need. You should also clean the pads of the brace regularly using soap and water.
You might consider applying 3M tape to the brace’s metal uprights and screws to prevent wear on his clothes.
And finally, do not lengthen or shorten the brace yourself. This can derail any progress made with the brace. Always have a professional make such adjustments.
Wind Down Brace Wearing
Once your child has reached skeletal maturity, she will likely be given the green light to shed the brace. At that point, she’ll likely want to go cold turkey and abandon the thoracic deformity brace altogether.
Don’t let that happen. Brace wearing should be wound down gradually and with careful monitoring. If the curve shows signs of worsening, your daughter may need to return to regular brace wearing.
How Successful Is Bracing for Kyphosis Hunchback Treatment?
Not everyone who undergoes bracing treatment achieves permanent correction of their hunchback condition. For some, the back reverts to its normal kyphosis/lordosis curve once brace-wearing ceases.
Success rates vary based on how early bracing was started, the degree of kyphosis and how well the patient stuck with the bracing regimen.
Scheuermann's Disease Surgery
Surgery for Scheuermann's kyphosis is an invasive procedure that comes with many risks, so it is certainly not a first choice for treating this spinal condition. It is generally only considered for patients with thoracic curves greater than 75 degrees and/or if the patient is also experiencing neurological problems or lives with major pain.
Adults with Scheuermann’s Disease might also consider reconstructive surgery if their symptoms are quite severe and disabling.
Besides being aware that there are a lot of risks that go along with this operation, you should also know that the goal of surgery is not to improve the cosmetic appearance of the curve. Rather it is to reduce the deformity and lessen any pain or neurological symptoms that come along with it.
What Does Surgery Entail?
Before going under the knife, a doctor will recommend an MRI to rule out any disc herniations or other issues that might put the spinal cord at risk during the procedure.
The operation itself involves a front thoracotomy that releases the tissues, removes the discs and places a bone graft in the spaces to fuse the thoracic spine. The surgeon may also approach the patient through the back to use hardware (rods, bars, wires, screws) to hold the spinal column straight as it fuses.
In all, the procedure typically takes four to five hours for most humans.
Scheuermann's Kyphosis Surgery Recovery
Advances in technology mean that surgery is far easier to recover from now than it was before. You can generally plan on spending between three and seven days in the hospital following the procedure.
Post-surgery, a patient will be closely monitored by a physician and will be required to attend regular follow-up visits where healing and curve progression are monitored. In some cases, follow-up bracing may be needed. Plan for a four to six-week recovery period at home, according to Johns Hopkins Medicine.
The recovery process after this procedure is a fairly active one. As soon as a day after the procedure, the patient may be encouraged to get up and walk about. Movement can get the blood flowing, which is great for healing.
Physical therapy will likely be recommended on an outpatient basis following the surgery, along with an at-home exercise program. This will improve strength, flexibility, and range of motion.
Read more about what to expect after back surgery.
Post-surgery Results
Fusing the spine might sound a bit scary, but because this area of the spine does not typically move a lot, spinal fusion to this area has little affect on the normal motion or the spine and thus does not typically cause problems down the road.
If the surgery is successful, it can improve your child’s (or your own) quality of life by easing pain, improving self-image and improving the function of the spine.
But surgery is not always successful and the results are not always lasting. Around 5% of people who undergo this operation must receive a reoperation as soon as five years later.
Scheuermann’s Disease Prognosis
For most adolescents with kyphosis stemming from Scheuermann’s Disease, the pain passes once skeletal maturity is reached as your kid’s tissues will “get used to” the abnormal curve of the spine. Generally, the curve does not worsen once growth is complete, but it also does not improve.
Some with this condition will experience a reduced range of motion and ongoing posture issues.
Generally speaking, those who undergo bracing rather than surgery had more issues with body image and emotional well-being, while those who went under the knife had more pain.
Tips for Living with Scheuermann's Disease from Those Who’ve Been There
Know that if you or your child is suffering from Scheuermann’s kyphosis, you’re not alone. There are many forums and Scheuermann’s Disease support groups out there filled with advice, support, and information that you may not receive as a patient. These also offer a great avenue simply for venting about the challenges this condition poses.
Some of the tips I gleaned from such blogs and forums include the following:
- Change your posture at work—take regular breaks, rotate between standing and sitting, focus on engaging the core and using good posture.
- When working on a computer, tilt the screen and use a box for keyboard placement.
- Try Pilates with a reforming machine that targets the core.
- When seeing a physical therapist, be sure to see one who specializes in backs.
- Use a TENS unit to help with pain.
- Get deep tissue therapy/massage to relieve sore tissues.
- Take a hot shower with a massaging showerhead or spend some time in a sauna.
- Consider trigger-point injections.
- Try taking fish oil and/or a glucosamine sulfate (run this by your doctor first).